This white paper demonstrates the examinations we have made related to patient travelling and paper printing.
Executive summary
In January 2020, the NHS launched its campaign for delivering a Net Zero NHS. It outlined its objective to improve their carbon footprint and reduce the environmental impact of its services. Since then the NHS has embarked on a process to identify the most credible, ambitious date that the health service could reach net-zero emissions.
When we talk about digitised care pathways, we often look at the impact for patients and service providers. But it’s got a far wider positive impact to make - supporting the NHS on its own journey to achieving Net-Zero. To support this ambition, each NHS Health Trust or Board and Integrated Care System should have a Green Plan, setting out their aims, objectives, and delivery plans for carbon reduction.
In this white paper, we look at how digitised surgical, outpatient and care pathways can help the NHS to decarbonise patient journeys and understand the positive environmental impact that reduced patient travelling and paper printing can really have.
Additionally, with the flexibility digital communications provides, we get the double impact of staff being able to work from any location, cutting down on their travel. We haven’t defined that here, as the deployment of staff is very personal to each provider, but savings will be made overall.
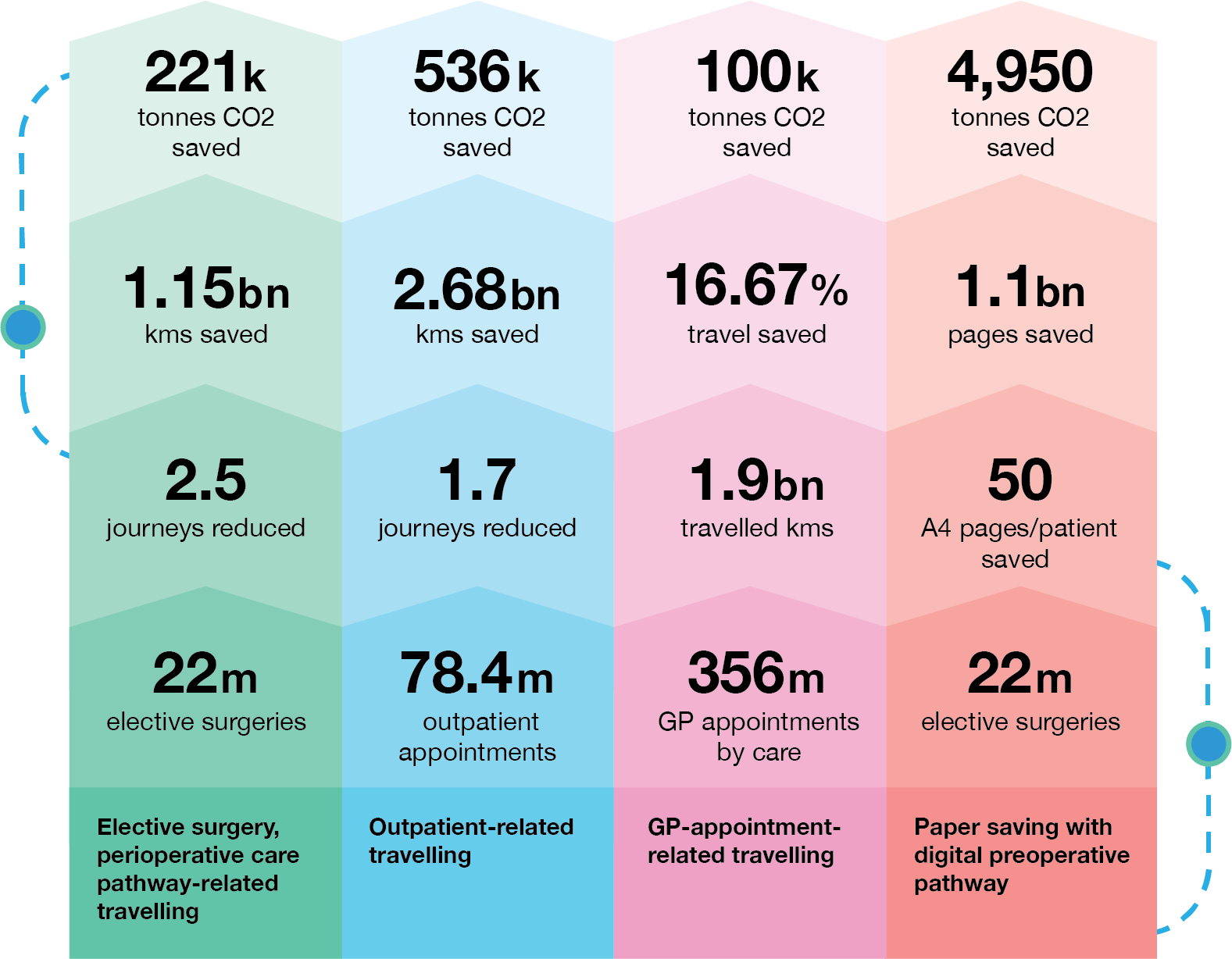
The following figures show the expansive effect using Buddy Healthcare's platform could have on the entire NHS.
Understanding the NHS’s Net-Zero objectives
![]() Emissions the NHS controls directly (their personal NHS Carbon Footprint)
Emissions the NHS controls directly (their personal NHS Carbon Footprint)
by 2040, with an ambition to reach an 80% reduction by 2028 to 2032![]() Emissions NHS can influence (NHS Carbon Footprint Plus)
Emissions NHS can influence (NHS Carbon Footprint Plus)
by 2045, with an ambition to reach an 80% reduction by 2036 to 2039
Source: Delivering a National Health Service, p. 5
The NHS is the largest employer in Britain, and it's responsible for around 4% of the nation's carbon emissions. A key component of the NHS’s make-up is the companies and suppliers it partners with - the supply chain. This makes the effort to support the NHS in the For a Greener NHS programme and contribute to achieving the target, a collaborative one, and means its supply chain can play a key role.
This paper presents calculations and examines how Buddy Healthcare’s care coordination platform improves the NHS's carbon footprint and reduces the environmental impact of its perioperative and other patient care pathway services.
In this white paper, we will look in more detail at how the NHS, partnering with Buddy Healthcare, can reduce its carbon emissions by reducing unnecessary travelling to places of care and back home and also avoiding paper printing that is currently required due to the manual and non-digital patient care processes. This also assists the NHS in its NHS@Home ambitions, where more remote care takes place and reliance on urgent care diminishes, with proactive healthcare. We are using a spreadsheet-based calculator throughout this white paper to demonstrate the calculations we have made.
Naturally, patients have to travel to a hospital on their surgery day, but by using the BuddyCare platform, we can significantly reduce preoperative and postoperative hospital visits. The BuddyCare care coordination platform can also help to drastically reduce outpatient visits as well as primary and community care visits through remote consultation, digital patient data collection and remote monitoring.
We believe that reducing patient travel will have a significant effect on carbon emissions, as well as digitising care processes, eliminating printing and mailing paper. Additionally, our in-built messaging and reminders eliminate the need for postage costs, which are now significant.
Executive Eight steps for the NHS - Three steps for Buddy Healthcare summary
The NHS has identified eight early steps that will be taken to decarbonise. These steps include care, medicines and supply chain, transport and travel, innovation, hospitals, heating and lighting, adaptation efforts and values and our governance. Here’s how Buddy Healthcare supports the NHS in three simple steps.
![]() Transport and travel
Transport and travel
Buddy Healthcare supports the transport and travelling steps by reducing the number of times surgery or outpatient patients need to visit the hospital pre and postoperatively or for treatment. We also offer surgical and outpatient teams the ability to work remotely and flexibly to assess and monitor patients from any location. We can also offer remote consultation and remote patient monitoring, for primary care and community health. So, as well as patient travel reductions, we also support reductions in staff travel between sites, as well as supporting remote working.
![]() Innovative models of care
Innovative models of care
Buddy Healthcare supports models of care and innovative steps by offering a new remote and patient digital care model for the NHS, reducing unnecessary travel. Patient pathway digitalisation also eliminates printing of up to 50 pages of paper per surgical patient. This could amount to over 1 billion pages across the NHS.
How can elective surgery-related and outpatient travel be minimised?
In the UK, the NHS handles, on average, 22 million elective surgical procedures per year as well as nearly 30 million outpatient appointments. Each surgery requires patients to travel to the hospital pre- and postoperatively, on average, four times. The average number of kilometres travelled to a hospital is 26.2 km. This means 2.2 bn kilometres are travelled annually in associated transport and travel for elective surgery, and 3.25bn kilometres for outpatients.
It would mean the patient travel associated with elective surgery, therefore, could account for as much as 5% of the carbon footprint of the NHS. Based on this insight, an understanding of the CO2 emissions per kilometre by car or taxi is 0.192 kgs, and an average of 26.2km per hospital appointment, which means that the CO2 emissions are 5.03kg per trip.
Patient and staff travel, as well as the supply chain, including procurement, have been considered as something the NHS has little control over. However, as we’ve highlighted, choosing your technology partners and suppliers can have an immediate impact.
The NHS has started requesting that suppliers submit green values white papers in the procurement and tendering processes. It’s one of the reasons we wanted to make available the figures and examine the impact the BuddyCare platform can make in CO2 reduction and its objectives.
Digital health and remote patient support services, such as Buddy Healthcare’s care coordination platform, can significantly help reduce the number of times patients need to visit the hospital.
The Buddy Healthcare's care coordination platform digitises patient pathways, enabling automated but personalised patient communication to our patients’ app, as well as forms and questionnaires to be completed and submitted from home. If a healthcare provider wishes, video and audio consultations can be integrated into the care pathway to allow even more remote care services. In addition, remote monitoring can also be supported through connected devices to mobile phones.
.png?width=1816&height=842&name=1%20(2).png)
Reducing 2.5 journeys per elective surgery patient with Buddy Healthcare's care coordination platform
Most journeys to the hospital are taken by car or taxi. According to the CQC and other sources, 80% of patients opt for their own car or taxi, indicating a preference for private transport over public transport. As previously mentioned, on average, a patient attending an elective surgery visits a hospital four times.
Insights provided by our partner hospitals suggest that many patients would prefer not to travel to the hospital for what could be unnecessary appointments, thereby saving money and avoiding time off work. A digital platform enabling remote pre-operative assessment and outpatient remote appointments is more efficient by saving patients and the NHS time, money, and it has a remarkable environmental impact.
As per our example, transforming patients’ perioperative pathways to digital via Buddy Healthcare’s platform can save up to 2.5 journeys to the hospital per patient (on average). With the support of a digital platform, patients make fewer car and taxi trips to the hospital, resulting in a significant reduction of CO2 emissions.
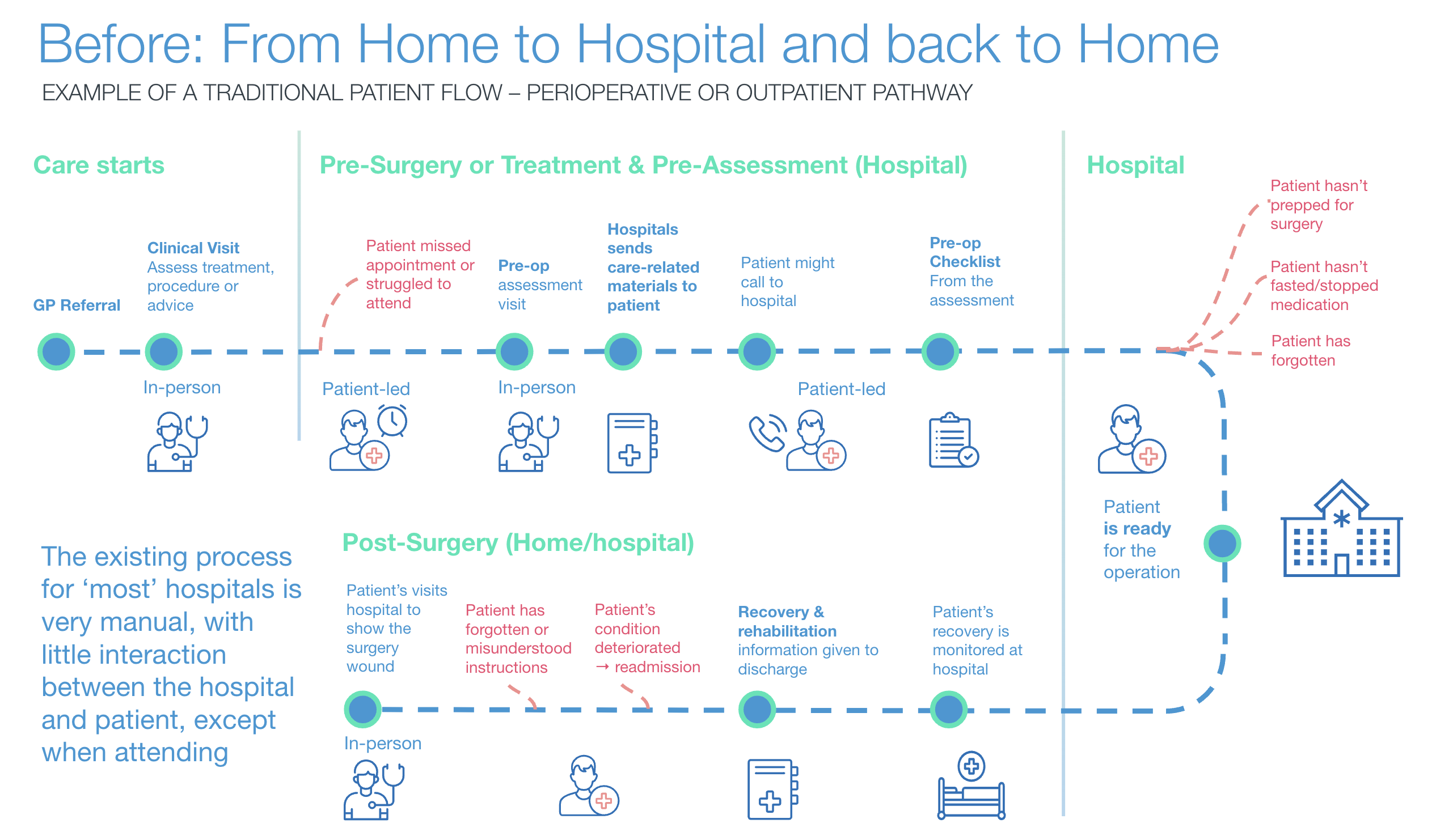
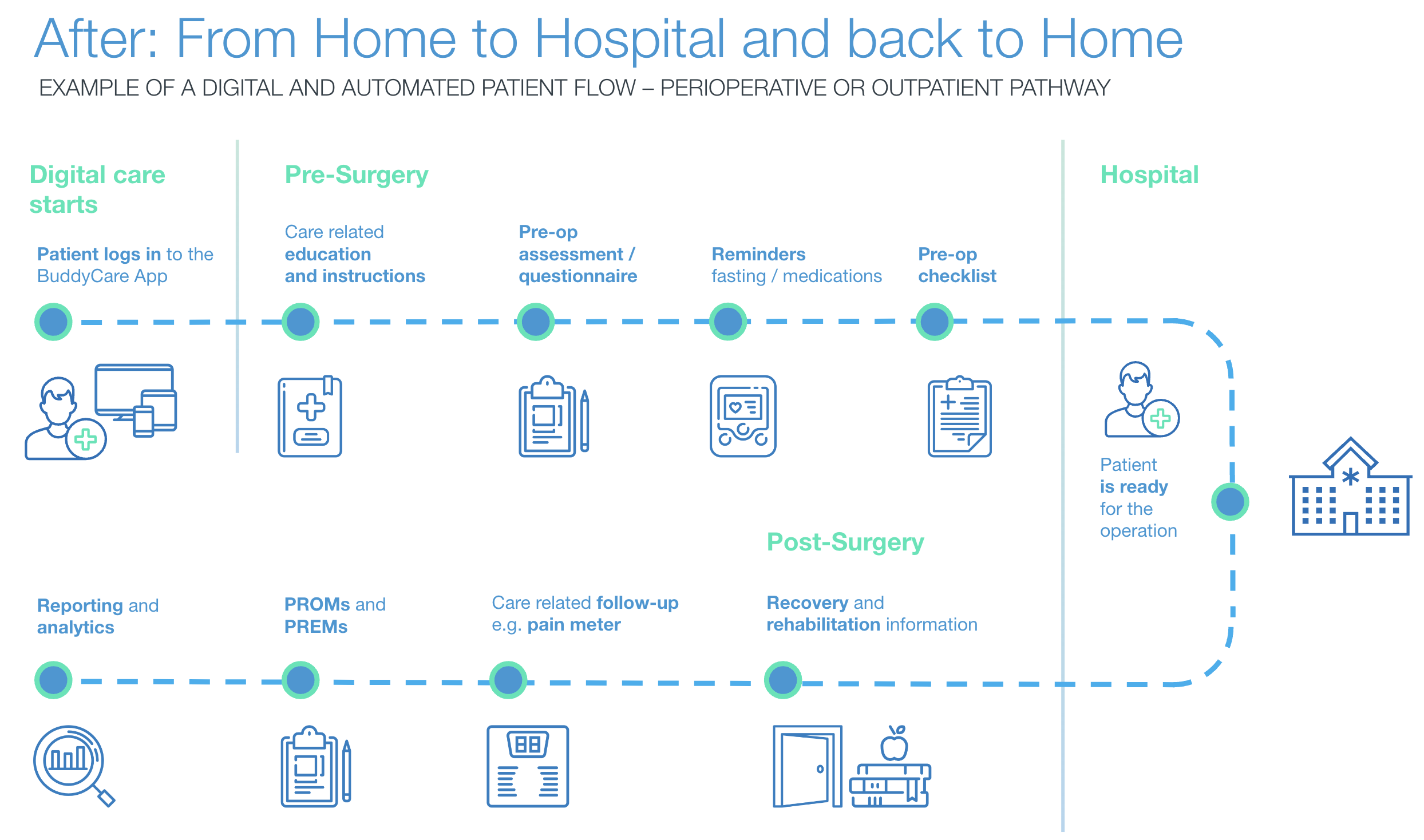
Pre-operative patient pathway - eliminates 1 or 2 visits to the hospital before surgery
Usually, patients preparing for surgery need to visit the hospital physically. Patients assigned to Buddy Healthcare's digital pre-operative care pathway are guided and educated through a pre-operative care process via a mobile app.
The process helps hospitals identify patients who don't need to visit the hospital before surgery. Most patients can submit digital pre-operative assessment forms from the comfort of their homes, eliminating one or two unnecessary visits or appointments to the hospital before surgery. The small number of patients who struggle with technology can use the “Acting on behalf” function and nominate a family member, carer, or advocate (or nurse) to help them, ensuring most patients can complete the pre-assessment form remotely. Switching to a digital process benefits both the NHS and its patients as it reduces the number of hospital appointments and travel leading up to surgery.
Post-operative patient pathway - eliminating 1 postoperative visit to the hospital
Usually, patients preparing for surgery need to visit the hospital physically. In the post-surgery phase of the digital surgical journey, patients are supported, monitored and managed remotely. The platform enables sharing of post-operative rehabilitation, medication and wound care instructions and reminders. It collects pain scales, patient-reported outcome and experience questionnaires, and allows patients to share their wound images from their mobile devices. Since the patients can share their well-being data and wound images safely with the care team from their mobile devices, many patients can avoid travelling to the hospital for these appointments.
At the same time, as patients are educated and patient data is gathered through the app, care teams can effectively monitor the patient flow remotely. They can assess patients' wound images, post-operative well-being questionnaires and recovery progress through the submitted photos and questionnaires. All this reduces the need for most patients to visit the hospital, and hospitals can transfer patients earlier onto a virtual ward as the platform allows well-being monitoring through gathered questionnaires.
We have found that, on average, one postoperative visit can be replaced by digital postoperative patient services and remote patient monitoring.
Scenario calculation: What if you could reduce perioperative care pathways-related journeys to the hospital from 4 to 2.5?
If each elective surgery patient in the UK travels to the hospital four times before and after surgery, it means 2.2billion travelling kilometres. In a scenario where all the patients would be assigned to the BuddyCare platform-supported digital perioperative care pathway, the number of times an elective surgery patient would need to visit the hospital would be reduced to 2.5.
The potential reductions show a possible total of 1.1bn kilometres saved in travel. This includes the calculation where 80% of the journeys are by car or taxi (excluding public or patient transport services). Furthermore, it means 221,337,600 kgs of savings and, in total, 211,338 tonnes of savings on carbon dioxide (CO2) emissions..png?width=1822&height=942&name=2%20(1).png)
Reducing printing - case example NHS Lanarkshire using BuddyCare
Preparing a patient for elective surgery requires a lot of manual care coordination work from the hospital, including printing and mailing care instructions. We are now using a real-world example here to describe how our customer, NHS Lanarkshire's pre-operative assessment process, became more sustainable through digital transformation and a reduction in printing.
In a typical pre-operative care process, like our customer’s NHS Lanarkshire’s pre-operative assessment process, the following information is delivered to the patient before surgery.
![]() Access specific hospital-based information, i.e. when arriving for surgery, how to find the surgery unit, or where to park
Access specific hospital-based information, i.e. when arriving for surgery, how to find the surgery unit, or where to park
![]() Digital pre-operative assessment form
Digital pre-operative assessment form
![]() Pre-habilitation information to inform the patient about “keeping fit for surgery”
Pre-habilitation information to inform the patient about “keeping fit for surgery”
![]() Instructions and reminders related to fasting and medicine reconciliation details
Instructions and reminders related to fasting and medicine reconciliation details
![]() Updates on any care process or appointment changes
Updates on any care process or appointment changes
The manual paper-based pre-operative assessment process didn’t only require patients to travel to the hospital physically to complete the pre-operative assessment. It also required printing all care and hospital-related instructions and mailing them to patients. A new digital pre-operative process with Buddy Healthcare’s platform enabled NHS Lanarkshire to digitally deliver all instructions, educational materials and questionnaires for all adult patients’ mobile devices. Before the digital pre-operative assessment process, NHS Lanarkshire printed, on average, 50 pages of paper for each patient attending a surgery.
Scenario calculation: What paper savings could be made if the pre-operative assessment process were digitised for all elective surgery patients in the UK?
Our calculations demonstrate that if all of the elective surgery patients in the UK (22 million) are printed 50 A4 pages per patient, only in the preoperative phase, that would be in total 1,1bn pages of printed paper. If using the most commonly used paper type of 80gsm computer printing paper, the total would be 200,000, and the number of tonnes of paper saved would be 5,500. That would result in 4.5g C02 savings in paper production, per A4 page, for a total of 4,950 tonnes of CO2 saved..png?width=1742&height=704&name=3%20(2).png)
Reducing the number of outpatient journeys per patient
We have previously touched on reducing perioperative travelling and pre-operative process-related paper printing. Since Buddy Healthcare was established in 2016, digitising and automating operative medical specialities care coordination has been our core service. Out of the 25 medical specialities we cover today, 14 are already other than surgery-related. As a next step, we aim to expand our automated care coordination to support primary care and integrated care services. Our care coordination platform helps the NHS to reduce a significant number of all care-related travelling, such as outpatient travelling.
Scenario calculation: What are the C02 savings if outpatient-related travelling is reduced by 30%
We have made CO2 calculations to examine the impact of reducing the entire outpatient-related patient travelling in the UK. The number of outpatient appointments in the UK is around 78.4 million, assuming an average of 4.5 per patient. We have evaluated that our platform can help the NHS reduce it to 2.8 journeys per patient, thus saving 1.7 journeys per patient, which gives us a total percentage of travel saved of 30%.
Again, if the average travelling kilometres from home to hospital is 25km and all of the 78.4 million outpatients travel to the hospital and home 4 times, it means 8.8bn kms will be travelled annually. With the 30% reduction in the patients’ travelling reductions, the travelled kilometres would decrease by 2.79 billion kilometres. That would lead to CO2 potential savings of 536k tonnes of savings on carbon dioxide (CO2) emissions.
.png?width=1572&height=612&name=4%20(3).png)
Supporting ICS by reducing the need to travel to GP appointments
Again, if the average travelling kilometres from home to hospital is 25km and all of the 78.4 million outpatients travel to the hospital and home 4 times, it means 8.8bn kms will be travelled annually. With the 30% reduction in the patients’ travelling, the travelled kilometres would decrease by 2.79 billion kilometres. That would lead to CO2 potential savings of 536k tonnes of savings on carbon dioxide (CO2) emissions.
Scenario calculation: What C02 savings could be achieved if GP-related travelling is reduced by 16.67%
The average number of annual GP appointments in the UK is around 360 million, from which some are estimated to be virtual appointments. According to the NHS, the average travel by car to the GP is 5.5km and if all 356 million physical GP visits we estimated were travelled by car, it would mean a total of 1.9bn travelled kilometres. We have estimated that with the Buddy Healthcare care coordination platform’s seamless data movement from primary care to secondary care, in-app questionnaires/forms collections, video consultations and remote patient monitoring, then patient travelling to the GP appointment could be reduced by 16.67%. That would mean that more than 522 million kilometres could be saved. That would lead to CO2 potential savings of 100m kgs or, 100k tonnes carbon dioxide (CO2) emissions..png?width=1564&height=606&name=5%20(6).png)
Conclusions
The NHS – which makes up approximately 4% of the UK’s total carbon footprint – is aiming to reach Net Zero by 2045. If it is successful in its efforts, it could become the world’s first healthcare system to do so.
It stands to reason why it is focused on transforming across the board – from HR to IT – aligning with targets while also maintaining high-quality clinical care.
Its emissions as a direct result of indirect activity are one of the most significant and easily addressed areas for change, from the medical supply chain through to the way patients and workers get around, as well as the waste generated by unnecessary material usage.
The NHS will play a central role in the health emergency that climate change brings, so being able to take a leading role, positively impacting the path to Net Zero, is in its interests. It is clear that Net Zero and evidencing change will be embedded into everything the NHS and its suppliers and partners do, both now and in the future.
In this white paper, we looked in more detail at how working with a strategic partner like Buddy Healthcare can support the NHS in reducing patient and staff-related travelling, as well as paper printing and mailing.
We have used a spreadsheet-based calculator with reference numbers to calculate the following scenarios
The NHS – which makes up approximately 4% of the UK’s total carbon footprint – is aiming to reach Net Zero by 2045. If it is successful in its efforts, it could become the world’s first healthcare system to do so.
It stands to reason why it is focused on transforming across the board – from HR to IT – aligning with targets while also maintaining high-quality clinical care.![]() Reducing elective surgery-related patient travelling by 1.1bn kms.
Reducing elective surgery-related patient travelling by 1.1bn kms.![]() Eliminating perioperative pathway-related paper printing, reducing by 1.1bn.
Eliminating perioperative pathway-related paper printing, reducing by 1.1bn.![]() Reducing the number of outpatient journeys to the hospital by 30%
Reducing the number of outpatient journeys to the hospital by 30%![]() Supporting ICS in reducing the need for patients to travel to GP appointments by 16.67%
Supporting ICS in reducing the need for patients to travel to GP appointments by 16.67%
Do you want to hear more or discuss digitised patient pathways or carbon reduction? Please send us an email to info@buddyhealthcare.com .png?width=296&height=287&name=Asset%201%20(1).png)